Autoimmune Encephalitis | Vibepedia
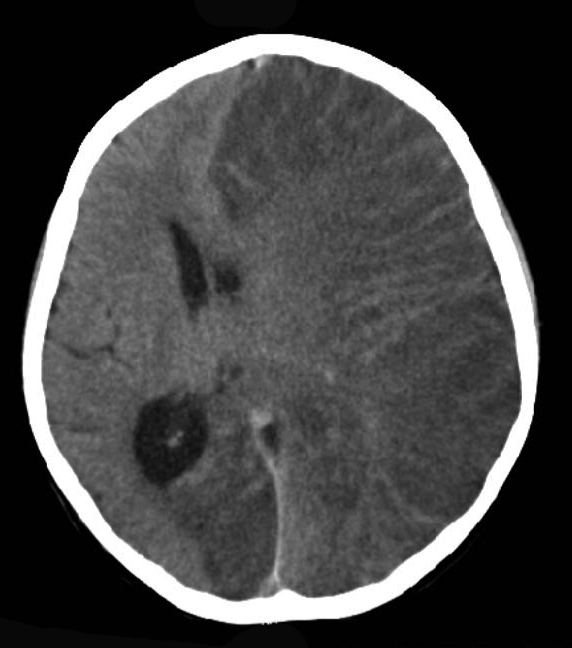
Autoimmune encephalitis (AIE) represents a critical class of non-infectious brain inflammation where the body's own immune system mistakenly targets neural…
Contents
- 🎵 Origins & History
- ⚙️ How It Works
- 📊 Key Facts & Numbers
- 👥 Key People & Organizations
- 🌍 Cultural Impact & Influence
- ⚡ Current State & Latest Developments
- 🤔 Controversies & Debates
- 🔮 Future Outlook & Predictions
- 💡 Practical Applications
- 📚 Related Topics & Deeper Reading
- Frequently Asked Questions
- References
- Related Topics
Overview
The concept of the immune system attacking the body's own tissues, now broadly termed autoimmunity, has a history stretching back to the late 19th century. Early observations of conditions like [[systemic-lupus-erythematosus|Systemic Lupus Erythematosus]] hinted at this internal conflict. However, the specific recognition of autoimmune encephalitis as a distinct entity is more recent, gaining traction in the late 20th century with advancements in immunology and neurology. Landmark studies began to identify specific autoantibodies targeting neural antigens, such as the [[nmdar-encephalitis|anti-NMDAR encephalitis]] first described in detail by [[josef-dalmau|Dr. Joseph Dalmau]] and colleagues in 2007. This discovery, linked to ovarian teratomas, revolutionized the understanding of AIE, shifting the paradigm from rare, obscure conditions to a more recognized and treatable spectrum of disorders. Prior to this, many cases were misdiagnosed as psychiatric disorders or infections, leading to delayed or inappropriate treatment.
⚙️ How It Works
Autoimmune encephalitis operates through a complex interplay of immune cells and autoantibodies targeting specific components of the central nervous system. The immune system, normally tasked with defending against foreign invaders, mistakenly identifies self-antigens on neurons or glial cells as threats. This can involve [[antibody-mediated-encephalitis|antibody-mediated]] attacks, where antibodies bind to receptors (like [[n-methyl-d-aspartate-receptor|NMDAR]] or [[ampareceptor|AMPAR]]) or ion channels on neuronal surfaces, disrupting synaptic function and leading to neuronal hyperexcitability or dysfunction. In other forms, T-cell mediated immunity may play a role, orchestrating inflammation and neuronal damage. The resulting neuroinflammation can cause cytotoxic edema, neuronal loss, and gliosis, manifesting as the diverse clinical symptoms observed. Treatment often involves suppressing this aberrant immune response through immunotherapies like [[corticosteroids|steroids]], [[intravenous-immunoglobulin|IVIg]], or [[plasma-exchange|plasma exchange]], and sometimes more targeted agents like [[rituximab|rituximab]] or [[cyclophosphamide|cyclophosphamide]].
📊 Key Facts & Numbers
Estimates suggest autoimmune encephalitis accounts for approximately 4% of all encephalitis cases, making it a significant cause of non-infectious brain inflammation. In adults, [[anti-nmdar-encephalitis|anti-NMDAR encephalitis]] is the most common type, identified in up to 4% of first-episode psychosis cases. Among children, it represents a leading cause of autoimmune-related neurological disorders. The incidence of AIE is estimated to be around 1.3 per 100,000 person-years, though this figure likely underestimates the true prevalence due to diagnostic challenges. Recovery rates vary widely; while around 75% of patients show improvement with treatment, approximately 25% may experience significant long-term sequelae or mortality. The economic burden is substantial, with prolonged hospitalizations and intensive care often required, potentially costing tens of thousands of dollars per patient.
👥 Key People & Organizations
Key figures in understanding autoimmune encephalitis include [[josef-dalmau|Dr. Joseph Dalmau]], whose work on [[anti-nmdar-encephalitis|anti-NMDAR encephalitis]] was pivotal. Other researchers like [[basil-peterson|Dr. Basil Petrides]] and [[ingrid-pfeiffer|Dr. Ingrid Pfeiffer]] have contributed significantly to characterizing various AIE subtypes and treatment protocols. Organizations such as the [[autoimmune-encephalitis-alliance|Autoimmune Encephalitis Alliance]] and the [[encephalitis-society|Encephalitis Society]] play crucial roles in raising awareness, supporting patients, and funding research. Major research institutions like the [[johns-hopkins-medicine|Johns Hopkins Medicine]] and [[mayo-clinic|Mayo Clinic]] are at the forefront of clinical trials and diagnostic advancements, developing new assays to detect a wider range of autoantibodies and refining treatment strategies. The collaborative efforts of neurologists, immunologists, and psychiatrists are essential in tackling this complex disease.
🌍 Cultural Impact & Influence
The cultural resonance of autoimmune encephalitis, while not as widespread as some other neurological conditions, is growing, particularly through patient advocacy and media portrayals. Stories of individuals experiencing sudden, dramatic shifts in personality and behavior, often initially misdiagnosed as psychiatric illness, highlight the profound impact of AIE. Documentaries and personal narratives shared on platforms like [[youtube-com|YouTube]] and [[reddit-com|Reddit]] have brought the lived experience of patients and their families to a broader audience. This increased visibility has fueled advocacy efforts, pushing for greater awareness among the public and medical professionals, and encouraging more research funding. The challenge of recognizing AIE, especially in its early, psychiatric-mimicking stages, remains a significant theme in these narratives, underscoring the need for better diagnostic tools and education.
⚡ Current State & Latest Developments
The current landscape of autoimmune encephalitis research is dynamic, with a strong focus on expanding the spectrum of known autoantibodies and refining treatment protocols. Recent developments include the identification of novel antibody targets, such as those against [[caspr2-antibody-encephalitis|CASPR2]] and [[leucine-rich-glioma-inactivated-1|LGI1]], which have distinct clinical profiles and treatment responses. Advances in [[high-throughput-screening|high-throughput screening]] technologies are accelerating the discovery of new autoantibodies. Furthermore, there's a growing emphasis on understanding the long-term outcomes and rehabilitation needs of AIE survivors, with ongoing studies examining cognitive deficits, psychiatric sequelae, and strategies for improving quality of life. The development of more precise immunotherapies, potentially targeting specific immune pathways with fewer side effects, is also a key area of investigation in 2024-2025.
🤔 Controversies & Debates
A significant controversy in autoimmune encephalitis revolves around the diagnostic criteria and the interpretation of antibody findings. While the presence of specific autoantibodies is highly suggestive, some patients exhibit clinical features consistent with AIE but lack detectable antibodies in standard serum or CSF tests, leading to debates about 'seronegative' AIE. Conversely, incidental detection of antibodies in asymptomatic individuals raises questions about their pathogenicity. Another debate centers on the optimal treatment duration and intensity, particularly for recurrent or refractory cases. The role of [[tumor-associated-autoimmunity|paraneoplastic syndromes]] in AIE also sparks discussion, with ongoing efforts to identify specific tumor markers and improve early cancer detection in affected patients. The classification and nomenclature of AIE subtypes themselves are also subject to refinement as new antibodies are discovered.
🔮 Future Outlook & Predictions
The future of autoimmune encephalitis management points towards greater precision and personalization. Researchers are actively developing [[liquid-biopsy|liquid biopsy]] techniques that could detect neural autoantibodies and biomarkers in blood, potentially enabling earlier and less invasive diagnosis. The exploration of novel immunomodulatory agents, including [[stem-cell-transplantation|stem cell transplantation]] and targeted B-cell depletion therapies, holds promise for refractory cases. Predictive models incorporating genetic predispositions, environmental triggers, and immune profiles are being developed to stratify risk and tailor treatment strategies. Furthermore, advancements in [[neuroimaging-techniques|neuroimaging techniques]] like diffusion tensor imaging (DTI) and functional MRI may offer more sensitive ways to track disease progression and treatment response. The ultimate goal is to achieve complete recovery for a higher percentage of patients, minimizing long-term neurological and psychiatric deficits.
💡 Practical Applications
Practical applications of understanding autoimmune encephalitis are primarily clinical, focusing on diagnosis and treatment. For clinicians, recognizing the diverse and often psychiatric-mimicking symptoms is paramount for timely referral to neurology and immunology specialists. Diagnostic tools include [[encephalography|EEG]] to detect seizure activity, [[magnetic-resonance-imaging|MRI]] to visualize brain inflammation, and crucially, [[cerebrospinal-fluid-analysis|CSF analysis]] and serum testing for specific autoantibodies. Treatment strategies, as mentioned, involve immunotherapies like [[corticosteroids|steroids]], [[intravenous-immunoglobulin|IVIg]], and [[plasma-exchange|plasma exchange]], often requiring hospitalization and intensive monitoring. Identifying and treating any underlying trigger, such as a tumor, is also a critical application. For patient advocacy groups, practical applications include developing educational materials for the public and healthcare providers, and supporting research initiatives.
Key Facts
- Year
- Late 20th Century (recognition)
- Origin
- Global
- Category
- science
- Type
- topic
Frequently Asked Questions
What are the most common symptoms of autoimmune encephalitis?
Symptoms of autoimmune encephalitis are highly variable and can develop rapidly over weeks. Common manifestations include behavioral and psychiatric changes such as paranoia, hallucinations, or catatonia, alongside neurological deficits like seizures, movement disorders (e.g., dyskinesias), memory loss, and autonomic dysfunction (e.g., heart rate or blood pressure irregularities). The presentation can often mimic psychiatric disorders, making early diagnosis challenging. Specific antibody types are associated with particular symptom clusters, for instance, [[anti-nmdar-encephalitis|anti-NMDAR encephalitis]] frequently presents with psychosis and seizures.
How is autoimmune encephalitis diagnosed?
Diagnosis of autoimmune encephalitis involves a combination of clinical evaluation, neurological examination, and laboratory testing. Neuroimaging, particularly [[magnetic-resonance-imaging|MRI]], is used to detect brain inflammation, though findings can be subtle or absent in early stages. [[Electroencephalography|EEG]] can reveal abnormal brain electrical activity, such as seizures. The definitive diagnosis often relies on detecting specific autoantibodies in the [[cerebrospinal-fluid-analysis|cerebrospinal fluid (CSF)]] or blood serum, targeting neuronal surface antigens or intracellular proteins. Tests for [[anti-nmdar-encephalitis|anti-NMDAR]], [[anti-lgi1-encephalitis|anti-LGI1]], [[anti-caspr2-encephalitis|anti-CASPR2]], and [[anti-gaba-b-receptor-encephalitis|anti-GABA-B receptor]] antibodies are standard. Identifying and treating any underlying trigger, such as a tumor, is also a critical diagnostic step.
What is the prognosis for autoimmune encephalitis?
The prognosis for autoimmune encephalitis varies significantly depending on the specific antibody type, the promptness of diagnosis and treatment, and the patient's overall health. While many patients, particularly those with [[anti-nmdar-encephalitis|anti-NMDAR encephalitis]], can achieve substantial recovery with early and aggressive immunotherapies like [[corticosteroids|steroids]] and [[intravenous-immunoglobulin|IVIg]], approximately 25% may experience severe long-term deficits or mortality. Some individuals may require ongoing rehabilitation for cognitive, psychiatric, or motor impairments. Recurrence is possible in some forms of AIE, necessitating long-term monitoring and potentially maintenance immunosuppression. Factors like age, presence of a tumor, and specific antibody titers can influence outcomes.
Can autoimmune encephalitis be cured?
While autoimmune encephalitis cannot always be 'cured' in the sense of complete eradication of the underlying autoimmune process, it is often treatable, leading to significant recovery. The primary goal of treatment is to suppress the aberrant immune response attacking the brain and to manage symptoms. Immunotherapies such as [[corticosteroids|steroids]], [[intravenous-immunoglobulin|IVIg]], [[plasma-exchange|plasma exchange]], and agents like [[rituximab|rituximab]] aim to reduce inflammation and clear autoantibodies. For [[anti-gaba-b-receptor-encephalitis|anti-GABA-B receptor]] and [[anti-nmdar-encephalitis|anti-NMDAR]] encephalitis associated with teratomas, surgical removal of the tumor can lead to dramatic improvement. For some patients, the disease can go into remission, but long-term monitoring is often necessary due to the potential for relapse.
What is the difference between autoimmune encephalitis and infectious encephalitis?
The fundamental difference lies in the cause: infectious encephalitis is caused by a pathogen, such as a virus (e.g., [[herpes-simplex-virus|herpes simplex virus]]) or bacteria, directly invading and inflaming the brain. Autoimmune encephalitis, on the other hand, is triggered by the body's own immune system mistakenly attacking healthy brain cells. While infections can sometimes precipitate autoimmune responses (post-infectious autoimmunity), the direct cause of damage in AIE is the immune system itself, not the pathogen. Treatment differs significantly; infectious encephalitis requires antiviral or antibiotic medications, whereas autoimmune encephalitis is treated with immunosuppressive therapies.
How can I support someone with autoimmune encephalitis?
Supporting someone with autoimmune encephalitis involves a multifaceted approach that addresses their physical, emotional, and cognitive needs. Patience and understanding are crucial, as symptoms can be unpredictable and include personality changes or confusion. Educate yourself about the specific type of AIE they have and its potential course. Assist with daily tasks, appointments, and medication adherence, as cognitive impairments can make these difficult. Encourage engagement in rehabilitation therapies, such as physical, occupational, and speech therapy, as recommended by their medical team. Provide emotional support by listening without judgment and helping them connect with support groups like the [[autoimmune-encephalitis-alliance|Autoimmune Encephalitis Alliance]]. Advocate for their needs with healthcare providers and ensure they have a safe and supportive living environment.
What are the latest research frontiers in autoimmune encephalitis?
Current research is heavily focused on identifying new autoantibody targets to improve diagnostic accuracy and expand the spectrum of known AIE types. Scientists are also investigating the precise mechanisms by which autoantibodies damage neurons, aiming to develop more targeted immunotherapies with fewer side effects than broad immunosuppression. Efforts are underway to develop better biomarkers for early diagnosis and prognosis, potentially through [[liquid-biopsy|liquid biopsies]]. Furthermore, research is exploring the role of [[gut-microbiome|gut microbiome]] alterations and genetic predispositions in the development of AIE, as well as refining strategies for managing long-term sequelae and improving rehabilitation outcomes for survivors. The development of AI-driven diagnostic tools for analyzing complex clinical and imaging data is also a growing area.