Herpes Simplex Virus | Vibepedia
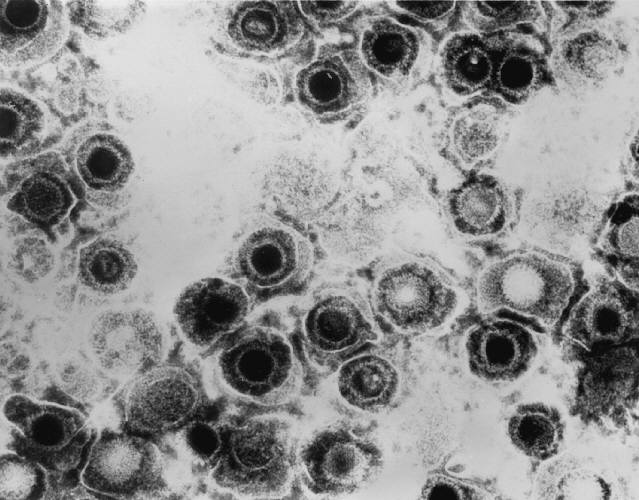
Herpes simplex virus (HSV), specifically HSV-1 and HSV-2, are two highly prevalent human viruses belonging to the [[Herpesviridae|Herpesviridae]] family…
Contents
- 🎵 Origins & History
- ⚙️ How It Works
- 📊 Key Facts & Numbers
- 👥 Key People & Organizations
- 🌍 Cultural Impact & Influence
- ⚡ Current State & Latest Developments
- 🤔 Controversies & Debates
- 🔮 Future Outlook & Predictions
- 💡 Practical Applications
- 📚 Related Topics & Deeper Reading
- Frequently Asked Questions
- References
- Related Topics
Overview
The history of herpes simplex virus is deeply intertwined with humanity's understanding of disease. While the characteristic lesions have been recognized since antiquity – with the term 'herpes' derived from the Greek word 'herpein,' meaning 'to creep' – the specific viral agents were not identified until the 20th century. Early descriptions by physicians like [[Hippocrates|Hippocrates]] in the 5th century BCE noted the recurrent nature of the sores. It wasn't until 1919 that [[Augustin-Jean|Augustin-Jean]] and T. Smith definitively linked a viral cause to herpes lesions. Later, in the 1960s, researchers like [[Werner & Ulbrich|Werner and Ulbrich]] distinguished between HSV-1, primarily associated with oral infections, and HSV-2, linked to genital infections, a classification that remains fundamental to clinical understanding and treatment strategies today. The discovery of [[acyclovir|acyclovir]] in the 1970s by [[Gertrude B. Elion|Gertrude B. Elion]] and George Hitchings marked a significant turning point in managing HSV symptoms.
⚙️ How It Works
Herpes simplex viruses are enveloped, double-stranded DNA viruses that operate through a well-defined replication cycle. Upon entry into a host cell, typically via [[glycoproteins|glycoprotein]]-mediated fusion with the cell membrane, the viral DNA is transported to the nucleus. Here, it hijacks the host cell's machinery to transcribe viral genes and replicate its own genome. HSV possesses a remarkable ability to establish lifelong latent infections by residing in [[ganglion|ganglia]] – clusters of nerve cells – such as the [[trigeminal ganglion|trigeminal ganglia]] for HSV-1 and the [[sacral ganglia|sacral ganglia]] for HSV-2. Reactivation, triggered by factors like stress, sunlight, or immune suppression, leads to viral replication and transport back to the periphery, causing recurrent outbreaks. The virus achieves immune evasion through various mechanisms, including the downregulation of [[MHC class I|MHC class I]] expression on infected cells.
📊 Key Facts & Numbers
The sheer scale of herpes simplex virus infection is staggering. Globally, it's estimated that approximately 3.7 billion people under the age of 50, or 67%, were infected with HSV-1 as of 2016, according to the [[World Health Organization|World Health Organization (WHO)]]. HSV-2 prevalence is lower but still significant, affecting an estimated 13% of the global population aged 15-49, translating to over 267 million people. In the United States alone, about 11.9% of individuals aged 14 to 49 had genital herpes in the period 2015-2016, with HSV-1 increasingly accounting for a portion of these genital infections. The economic burden is also substantial, with billions spent annually on managing outbreaks, treatments, and associated complications like [[herpes keratitis|herpes keratitis]] and [[neonatal herpes|neonatal herpes]].
👥 Key People & Organizations
Key figures in understanding and combating herpes simplex virus include [[Werner & Ulbrich|Werner and Ulbrich]], who first differentiated HSV-1 and HSV-2. [[Gertrude B. Elion|Gertrude B. Elion]] and George Hitchings, Nobel laureates, were instrumental in developing [[acyclovir|acyclovir]], the first effective antiviral treatment for HSV. Organizations like the [[World Health Organization|World Health Organization (WHO)]] play a crucial role in global surveillance and public health recommendations, while institutions like the [[Centers for Disease Control and Prevention|Centers for Disease Control and Prevention (CDC)]] in the U.S. provide vital data and guidance. Pharmaceutical companies such as [[GlaxoSmithKline|GlaxoSmithKline]] (developer of acyclovir) and [[Merck & Co.|Merck & Co.]] (developer of [[valacyclovir|valacyclovir]] and [[famciclovir|famciclovir]]) have been central to antiviral drug development. Ongoing research is also driven by academic institutions worldwide, including [[Johns Hopkins University|Johns Hopkins University]] and [[Stanford University School of Medicine|Stanford University]].
🌍 Cultural Impact & Influence
Herpes simplex virus has profoundly shaped human culture and social interactions, often carrying a significant [[social stigma|social stigma]] due to its association with STIs. The visible manifestation of cold sores or genital lesions has been a recurring motif in art and literature, symbolizing vulnerability, disease, and sometimes, forbidden desire. Public health campaigns, particularly those targeting STIs, have attempted to destigmatize HSV, emphasizing its prevalence and the importance of safe practices. The virus's impact extends to reproductive health, with concerns about transmission during childbirth leading to specific medical protocols. Furthermore, the ongoing search for a cure or a highly effective vaccine has fueled a persistent narrative of scientific challenge and hope within popular culture and medical discourse, influencing perceptions of viral infections more broadly.
⚡ Current State & Latest Developments
The current landscape of herpes simplex virus management is characterized by effective antiviral therapies that control outbreaks but do not eradicate the virus. Recent developments include research into [[therapeutic vaccines|therapeutic vaccines]] aimed at reducing viral shedding and symptom severity, rather than purely preventative ones. Studies are exploring novel drug delivery systems and combination therapies to enhance efficacy and patient adherence. There's also a growing focus on understanding the asymptomatic shedding of the virus, which accounts for a significant portion of transmission, and developing diagnostic tools to better detect it. The [[National Institute of Allergy and Infectious Diseases|National Institute of Allergy and Infectious Diseases (NIAID)]] continues to fund significant research into HSV pathogenesis and potential cures, with promising preclinical results emerging from various [[biotechnology companies|biotechnology companies]] and academic labs.
🤔 Controversies & Debates
The controversies surrounding herpes simplex virus often revolve around [[stigma and disclosure|stigma and disclosure]]. Many individuals diagnosed with HSV struggle with the psychological burden and the decision of when and how to disclose their status to partners, leading to debates about the ethics and social implications of living with a chronic, incurable infection. Another area of contention is the varying prevalence rates across different demographics and geographic regions, prompting discussions about health disparities and access to care. Furthermore, the ongoing debate about whether HSV-1 should be classified solely as an oral infection or recognized more broadly as a cause of genital herpes continues to influence public health messaging and diagnostic approaches. The development of new treatments also sparks debate regarding accessibility and cost-effectiveness.
🔮 Future Outlook & Predictions
The future outlook for herpes simplex virus is one of cautious optimism, driven by advancements in [[virology|virology]] and immunology. The ultimate goal remains a functional cure or a highly effective vaccine that can prevent both infection and transmission. Researchers are exploring gene-editing technologies like [[CRISPR-Cas9|CRISPR-Cas9]] to target latent viral reservoirs within neurons. Additionally, the development of [[mRNA vaccine technology|mRNA vaccine technology]], popularized by [[Pfizer-BioNTech|Pfizer-BioNTech]] and [[Moderna|Moderna]]'s COVID-19 vaccines, is being adapted for HSV, with several candidates in clinical trials. Success in these areas could dramatically alter the global burden of HSV, reducing transmission rates, alleviating symptoms, and significantly diminishing the associated social stigma. Projections suggest that a breakthrough vaccine or cure could emerge within the next 10-15 years, though challenges in targeting latent viruses persist.
💡 Practical Applications
While there is no cure, practical applications of current knowledge focus on symptom management and prevention. Antiviral medications like [[acyclovir|acyclovir]], [[valacyclovir|valacyclovir]], and [[famciclovir|famciclovir]] are widely prescribed to reduce the frequency, duration, and severity of outbreaks. Patient education on trigger avoidance (e.g., stress management, sun protection) is a key component of management. For individuals with frequent or severe outbreaks, suppressive therapy can be a highly effective long-term strategy. Public health initiatives focus on promoting safe sex practices, including [[condom use|condom use]], to reduce transmission, although condoms do not offer complete protection as they may not cover all infected areas. Diagnostic tests, including [[PCR testing|PCR testing]] and antibody blood tests, are crucial for accurate diagnosis and management by healthcare providers.
Key Facts
- Year
- 20th Century (identification of distinct types)
- Origin
- Global
- Category
- science
- Type
- concept
Frequently Asked Questions
What are the main differences between HSV-1 and HSV-2?
While both are herpes simplex viruses, HSV-1 is traditionally associated with oral infections (cold sores) and HSV-2 with genital infections. However, oral sex has led to a significant increase in HSV-1 genital infections, blurring these lines. HSV-1 typically establishes latency in the [[trigeminal ganglion|trigeminal ganglion]], while HSV-2 usually resides in the [[sacral ganglia|sacral ganglia]]. Both can cause symptoms in either location, and both establish lifelong latent infections.
How is herpes simplex virus transmitted?
HSV is transmitted through direct contact with an infected person's sores, saliva, or genital secretions during periods of viral shedding. This shedding can occur even when no visible sores are present, making asymptomatic transmission a significant factor. Transmission can happen through kissing, oral sex, vaginal sex, and anal sex. Sharing personal items like razors or towels can also transmit HSV-1 if they come into contact with infected bodily fluids.
Can herpes simplex virus be cured?
Currently, there is no cure for herpes simplex virus. Once infected, the virus remains dormant in the body's nerve cells and can reactivate periodically. However, antiviral medications such as [[acyclovir|acyclovir]], [[valacyclovir|valacyclovir]], and [[famciclovir|famciclovir]] can effectively manage outbreaks by reducing their frequency, duration, and severity. These medications do not eliminate the virus from the body but significantly improve the quality of life for infected individuals.
What are the long-term health implications of HSV infection?
For most individuals, HSV infections are a source of discomfort and social stigma rather than severe health risks. However, complications can arise, particularly in immunocompromised individuals. These can include [[herpes simplex encephalitis|herpes simplex encephalitis]] (a dangerous brain infection), [[herpes keratitis|herpes keratitis]] (affecting the eye and potentially causing blindness), and [[neonatal herpes|neonatal herpes]] (a severe, potentially fatal infection in newborns transmitted during childbirth). HSV-2 infection also increases the risk of acquiring [[HIV infection|HIV infection]].
Why is HSV still so prevalent despite available treatments?
HSV's high prevalence is due to several factors: asymptomatic shedding means many people are unaware they are infected and can transmit it; the virus establishes lifelong latency, making eradication impossible with current therapies; and the social stigma often discourages open discussion and testing. Furthermore, while treatments manage symptoms, they don't prevent transmission entirely, and preventative vaccines have yet to achieve widespread success, though research is ongoing.
How can I reduce the risk of contracting or spreading herpes simplex virus?
Reducing the risk involves practicing safer sex, including consistent [[condom use|condom use]], although condoms do not offer complete protection as they may not cover all infected areas. Open communication with sexual partners about [[STI status|STI status]] is crucial. Avoiding intimate contact during active outbreaks is essential. For individuals with HSV, taking prescribed antiviral medication for suppressive therapy can significantly reduce viral shedding and the risk of transmission to partners. Maintaining a strong immune system through healthy lifestyle choices may also help reduce outbreak frequency.
What is the future of herpes simplex virus treatment and prevention?
The future holds promise for improved HSV management and potential cures. Research is actively pursuing [[therapeutic vaccines|therapeutic vaccines]] designed to boost the immune system's ability to control the virus and reduce shedding. [[Gene therapy|Gene therapy]] approaches, including [[CRISPR-Cas9|CRISPR-Cas9]], are being investigated to target and eliminate latent virus from nerve cells. [[mRNA vaccine technology|mRNA vaccine technology]] is also being adapted for HSV, with several candidates in clinical trials aiming for prevention or significant symptom reduction. A functional cure remains the ultimate goal, with breakthroughs potentially within the next decade.