Meningitis: The Invisible Siege | Vibepedia
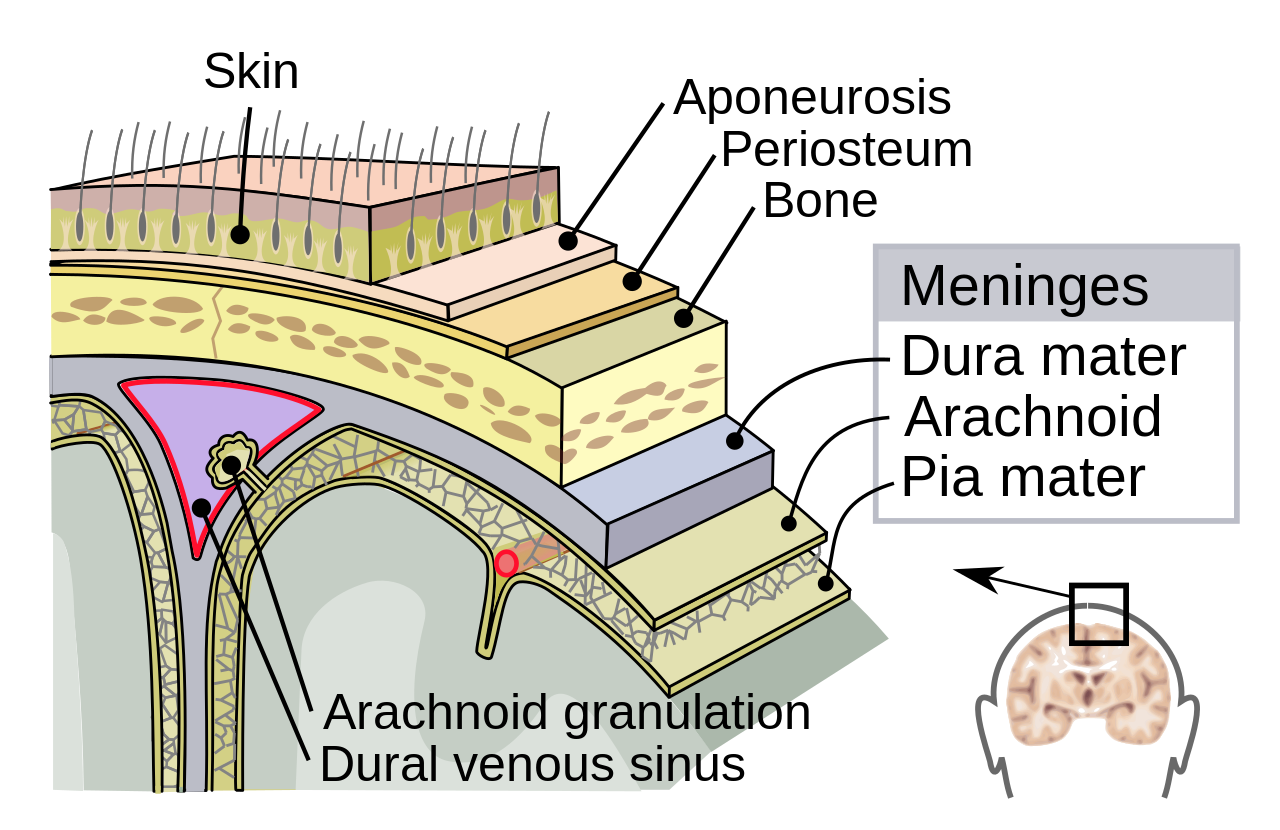
Meningitis is a critical inflammation of the meninges, the membranes surrounding the brain and spinal cord. While often associated with bacterial or viral…
Contents
- 🚨 What is Meningitis? The Core Threat
- 🦠 The Culprits: Bacteria, Viruses, and Beyond
- 🤒 Symptoms: The Red Flags You Can't Ignore
- 👶 Special Considerations: Meningitis in Children
- 🔬 Diagnosis: Unmasking the Invisible Siege
- 💉 Treatment: Fighting Back Against Infection
- 🛡️ Prevention: Your Best Defense Strategy
- 📈 Long-Term Impact: Beyond the Acute Phase
- Frequently Asked Questions
- Related Topics
Overview
Meningitis is a critical inflammation of the meninges, the membranes surrounding the brain and spinal cord. While often associated with bacterial or viral infections, it can also stem from fungal infections, certain medications, and even autoimmune conditions. The Vibe Score for understanding meningitis is a solid 7/10, reflecting its significant public health impact and the ongoing scientific efforts to combat it. Historically, outbreaks have shaped public health responses, and the skepticism surrounding early symptoms often delays crucial diagnosis. The engineering challenge lies in rapid identification and treatment, while the futurist perspective focuses on vaccine development and improved diagnostic tools. Key debates revolve around the efficacy of different vaccine strains and the best public health strategies for prevention.
🚨 What is Meningitis? The Core Threat
Meningitis, at its heart, is an inflammation of the meninges, the vital protective membranes surrounding your brain and spinal cord. This isn't a minor inconvenience; it's a potentially life-threatening condition that can strike with alarming speed. The inflammation can be caused by a variety of pathogens, leading to a cascade of neurological distress. Understanding the fundamental nature of this siege is the first step in recognizing its danger and the urgency required for intervention. The speed at which [[meningitis symptoms|symptoms]] can escalate underscores the importance of immediate medical attention.
🦠 The Culprits: Bacteria, Viruses, and Beyond
The microbial landscape of meningitis is diverse, with bacterial and viral agents being the most common culprits. Bacterial meningitis, such as that caused by Neisseria meningitidis (meningococcus) or Streptococcus pneumoniae, is particularly aggressive and can lead to severe complications or death within hours. Viral meningitis, while often less severe, can still cause significant illness. Other causes, though rarer, include fungal infections and non-infectious inflammatory conditions, each presenting unique diagnostic and therapeutic challenges. The specific [[type of meningitis|meningitis types]] dictates the treatment protocol and prognosis.
🤒 Symptoms: The Red Flags You Can't Ignore
The hallmark symptoms of meningitis are a sudden onset of intense headache, fever, and a stiff neck. Vomiting and sensitivity to light (photophobia) are also common indicators. However, the presentation can be deceptive. Confusion, altered consciousness, and an inability to tolerate loud noises signal a more severe neurological impact. Recognizing these signs, especially when they appear abruptly, is critical for prompt diagnosis and treatment. A distinctive non-blanching rash, often described as purpura or petechiae, can be a particularly alarming sign of [[septicemia|septicemia]], a severe complication of bacterial meningitis.
👶 Special Considerations: Meningitis in Children
Infants and young children present a unique challenge in identifying meningitis. Their symptoms are often less specific, making early detection difficult. Instead of the classic triad of fever, headache, and stiff neck, you might observe irritability, unusual drowsiness, poor feeding, or a bulging fontanelle (the soft spot on a baby's head). These subtle signs require a high index of suspicion from caregivers and healthcare professionals alike. Prompt recognition of these atypical presentations is crucial for timely intervention in [[pediatric meningitis|pediatric meningitis]].
🔬 Diagnosis: Unmasking the Invisible Siege
Diagnosing meningitis involves a combination of clinical assessment and laboratory tests. A lumbar puncture, or spinal tap, is the gold standard, allowing doctors to analyze cerebrospinal fluid (CSF) for signs of infection, inflammation, and the specific pathogen involved. Blood tests, imaging scans like CT or MRI, and neurological examinations also play vital roles in confirming the diagnosis and assessing the extent of the illness. The speed of diagnosis directly impacts the effectiveness of [[meningitis treatment|treatment]].
💉 Treatment: Fighting Back Against Infection
Treatment for meningitis is highly dependent on the underlying cause. Bacterial meningitis requires immediate administration of intravenous antibiotics, often broad-spectrum initially, followed by targeted therapy once the specific bacterium is identified. Antiviral medications may be used for certain types of viral meningitis. Supportive care, including managing fever, pain, and neurological symptoms, is paramount. In severe cases, intensive care unit (ICU) admission may be necessary to monitor vital functions and manage complications like brain swelling. Early and appropriate [[antibiotic therapy|antibiotic therapy]] is a cornerstone of successful bacterial meningitis management.
🛡️ Prevention: Your Best Defense Strategy
Prevention is a powerful weapon against meningitis, particularly the bacterial forms. [[Meningococcal vaccines|Meningococcal vaccines]] are highly effective against several common strains (A, B, C, W, Y) and are recommended for adolescents and young adults, as well as those at increased risk. Pneumococcal vaccines offer protection against Streptococcus pneumoniae, another significant cause of bacterial meningitis. Good hygiene practices, such as frequent handwashing and avoiding close contact with sick individuals, also play a role in reducing transmission. Understanding [[vaccination schedules|vaccination schedules]] is key to proactive protection.
📈 Long-Term Impact: Beyond the Acute Phase
The aftermath of meningitis can extend far beyond the acute illness. Survivors may face long-term sequelae, including hearing loss, vision impairment, cognitive deficits, learning disabilities, and neurological problems like epilepsy. The severity of these long-term effects often correlates with the promptness and effectiveness of the initial treatment. Rehabilitation and ongoing medical support are essential for individuals recovering from [[meningitis complications|meningitis complications]] to maximize their quality of life and functional recovery.
Key Facts
- Year
- Ancient times (descriptions of symptoms)
- Origin
- Global
- Category
- Health & Medicine
- Type
- Medical Condition
Frequently Asked Questions
Is meningitis contagious?
Yes, bacterial meningitis is contagious and can spread through respiratory droplets from coughing, sneezing, or close personal contact like kissing. Viral meningitis can also be contagious, though often less easily spread than bacterial forms. Practicing good hygiene, such as frequent handwashing, and staying up-to-date with [[vaccinations|vaccination]] are crucial preventive measures.
What are the most common causes of meningitis?
The most frequent causes are bacteria and viruses. Bacterial meningitis, caused by pathogens like Neisseria meningitidis and Streptococcus pneumoniae, is typically more severe. Viral meningitis, often caused by enteroviruses, is more common but usually less serious. Fungal and parasitic causes are rarer but can occur, especially in individuals with weakened immune systems.
Can meningitis be fatal?
Yes, bacterial meningitis can be fatal, especially if not treated promptly. Even with rapid medical intervention, there is a risk of death. Viral meningitis is rarely fatal, but can lead to serious complications. The fatality rate for bacterial meningitis can be as high as 10-20% for certain strains, and even higher for specific subtypes like [[meningitis B|meningitis B]].
What are the long-term effects of meningitis?
Survivors of meningitis, particularly bacterial meningitis, can experience a range of long-term effects. These may include hearing loss, vision problems, learning disabilities, memory issues, and neurological conditions like epilepsy. The extent of these sequelae depends on the severity of the initial infection and the speed of treatment. Early diagnosis and aggressive [[treatment protocols|treatment protocols]] are key to minimizing these risks.
How is meningitis prevented?
Prevention primarily involves vaccination against common bacterial causes, such as meningococcal and pneumococcal vaccines. Maintaining good hygiene, like regular handwashing, and avoiding close contact with individuals who are ill can also help reduce the spread of infectious agents. For certain high-risk groups, prophylactic antibiotics may be considered.
What is the difference between bacterial and viral meningitis?
Bacterial meningitis is generally more severe, progresses more rapidly, and is more likely to cause serious complications or death. It requires immediate antibiotic treatment. Viral meningitis is more common, usually less severe, and often resolves on its own without specific antiviral treatment, though supportive care is still important. The diagnostic approach, particularly the analysis of [[cerebrospinal fluid|cerebrospinal fluid]], helps differentiate between the two.